When we think about personalized medicine, we often think of researchers designing therapies to match a person’s disease. Now researchers are looking at this the other way – matching people to a specific therapy.
“Historically, patients who have exhausted other options but are still reasonably well might access a clinical trial based on their cancer type, but without that new therapy being targeted to their tumor’s particular genetic profile,” said Dr. Matthew Krebs, the lead clinician of a Nature Medicine study. The study was funded by Cancer Research UK, AstraZeneca, The Christie NHS Foundation Trust and the NIHR Manchester Biomedical Research Center.
The principle of personalized medicine is to treat patients with highly targeted therapies that are specific to the patient’s condition so that the treatment plan can be optimally effective against their cancer. Currently, cancer patients are enrolled in clinical trials based on the type of cancer they have and some genetic information obtained from a tumor biopsy. However, patients might still end up in a one-size-fits-all kind of trial.
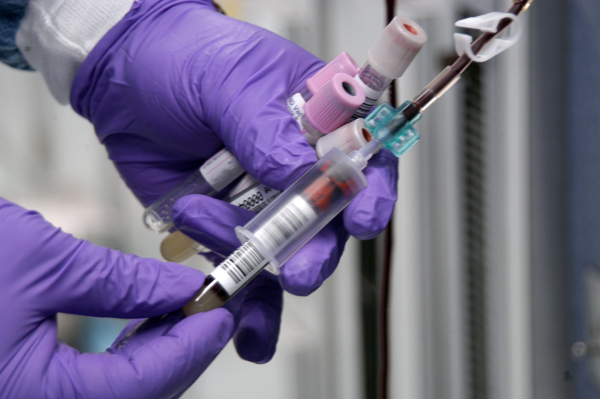
Liquid biopsies are blood tests that provide the same type of genetic information to an oncologist without invasive surgery. When coupled with advanced genetic sequencing techniques, a small sample of blood carrying circulating tumor DNA can tell scientists about the tumor type, specific mutations it carries and its potential to resist treatments. Moreover, liquid biopsies are more likely to reflect a patient’s current disease state since traditional tumor biopsies may be taken months in advance.
In the new article, the researchers found that the blood test was just as good as the tumor biopsy in detecting cancer-related mutations in a short timeframe. In 41 out of 100 patients with advanced cancer, the blood test revealed mutations that could be targeted with experimental drugs.
The researchers were able to match 11 patients to early-phase clinical trials which were testing treatments that fit their tumor’s genetic profile. One of those patients carrying a specific mutation in her lung tumor demonstrated a partial response to an experimental therapy and lived on for another year without disease progression. Overall, the test costs about £1,600 per patient.
These promising, early results offer new hope for patients with terminal cancers. The researchers are already working on the second part of their study, where 450 patients will undergo this matching system.
Professor Caroline Dive, the laboratory lead author of the study from the Cancer Research UK Manchester Institute said the team is working on improving the blood testing approach.
“We are making the test more sensitive and adding new elements to it in order to understand more about a patient’s disease,” she said. “We are also taking several blood samples over time to see if a faulty gene(s) is disappearing with treatment, or if there is emergence of a new genetic fault that could lead to treatment resistance. This would allow us to stop a failing treatment and consider new options to stay a step ahead of the disease.”
The value of using and sharing genetic data to match patients to experimental therapies made headlines when the Oncology Precision Network was founded in 2016. Up-to-date genetic information from liquid biopsies could be shared in a similar manner to help inform treatment decisions for various types of cancer.
While this new matching system cannot guarantee personalized treatment for all cancer patients, it may be worthwhile to know if there are treatments available that may offer a greater chance of survival.









Join or login to leave a comment
JOIN LOGIN