Researchers from the National Heart, Lung and Blood Institute of the National Institutes of Health (NIH) are back with a new study linking biologics treatment of the inflammatory skin disease, psoriasis, to reduced cardiovascular disease risk — only this time, they used a brand-new method to assess inflammation.
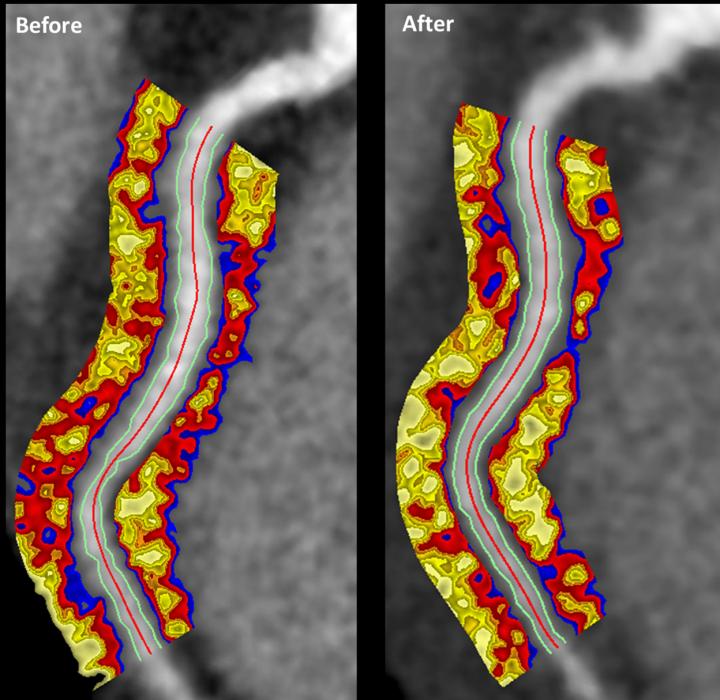
Senior author Dr. Nehal Mehta and his team measured changes in the composition of perivascular fat (fat surrounding arteries) as a biomarker of inflammation. This technique is known as perivascular fat attenuation index (FAI).
“FAI is a new method of analyzing CT scans that can predict a patient’s risk of fatal heart attacks and other cardiac events years in advance, and independent of other traditional risk factors for heart disease,” explained study co-author Dr. Charalambos Antoniades, professor of cardiovascular medicine at Oxford University.
This technique has been used to predict cardiovascular disease risk in the past, however, the authors say they’re the first to show a perivascular FAI response to anti-inflammatory treatments.
Out of 134 patients with psoriasis, 82 who received biologics treatment for one year had significant reductions in coronary inflammation as measured by perivascular FAI. The control group, who received standard topical or light therapy, had improvements in skin symptoms but did not show any changes to perivascular FAI. The study was published in JAMA Cardiology at the end of July.
RELATED VITALS: Lowering Coronary Heart Disease Risk in Psoriasis Patients
The group’s previous paper assessed coronary plaque buildup and measured inflammatory biomarkers in the blood to gauge if anti-inflammatory biologics would have an effect on coronary heart disease risk in patients with psoriasis. What they found was consistent with their hypothesis: biologics treatment led to improvements in psoriasis skin symptoms and reductions in total coronary plaque burden. Those results suggested that biologics treatment could lower the risk of coronary heart disease in patients with chronic inflammatory diseases like psoriasis.
It’s possible that not all biologic treatments have a positive effect on heart health. The American Academy of Dermatology lists adalimumab (Humira), etanercept (Enbrel) and infliximab (Remicade) as psoriasis treatments with heart-health benefits. All of these drugs block the inflammatory molecule, tumor necrosis factor (TNF). However, most biologics, including anti-TNFα, plus antibodies against various interleukin proteins have mixed effects on cardiovascular disease risk, according to a review published in Frontiers in Immunology.
With this new data, Dr. Mehta and his team provide further evidence that biologics treatment could lower a person’s risk of cardiovascular disease, not just in psoriasis, but other inflammatory conditions as well. Moreover, they now have a new technique to evaluate the effects of biologics treatment on coronary inflammation. Altogether, clinicians can use this information to potentially guide individualized treatment plans.








Join or login to leave a comment
JOIN LOGIN