Since the first medical device sterilization facility closure made headlines in April, the US Food and Drug Administration (FDA) has been quick to implement damage control. But now, it looks like the state of sterilization is spiraling: acting commissioner Dr. Ned Sharpless issued a statement last week warning manufacturers of potential nationwide shortages.
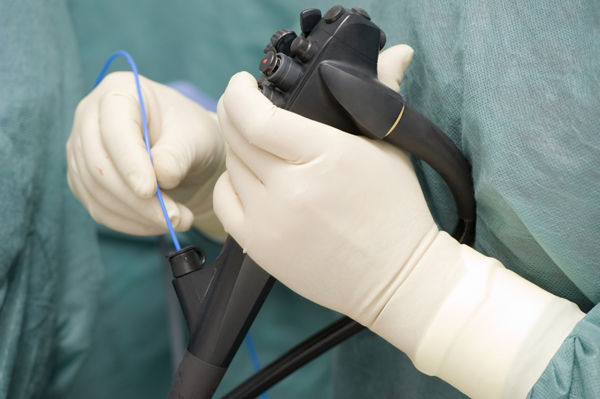
Ethylene oxide gas is routinely used to sterilize common medical devices, from surgical kits to feeding tubes to coronary stents, but this substance is also a recognized carcinogen. At this time, there is no feasible alternative to sterilize half of the US’s medical devices, meaning any disruption to sterilization could impact the supply to hospitals and patients.
Problems for device manufacturers really began when the Illinois Sterigenics facility was ordered to cease ethylene oxide sterilization until it installed new emissions capture and control systems that must be approved by the Illinois Environmental Protection Agency (IEPA), as described in a state-issued Seal Order. A frequent patron of Sterigenics Willowbrook quickly found themselves struggling in the wake of the closure, announcing a temporary shortage of pediatric breathing tubes less than a week after the news broke. Despite whispers of re-opening the facility, Sterigenics announced it will not reopen its doors in October.
RELATED: How to Choose the Best Sterilization Method for Your Medical Device
News of the Illinois plant closure ramped up investigations by the Environmental Protection Division (EPD) in Georgia, where concerns of ethylene oxide emissions by a Cobb County-based Sterigenics plant and Covington-based Becton Dickinson (BD) plant were on the rise. Sterigenics voluntarily suspended its sterilization operations to accelerate the installation of technology enhancements to its Atlanta facility. On Monday, BD was ordered to temporarily close its doors for a week, following a restraining order filed by the state of Georgia last Friday.
“Because the number of ethylene oxide contract sterilization facilities in the US is limited, we are very concerned that additional facility closures could severely impact the supply of sterile medical devices to health care delivery organizations that depend on those devices to take care of patients,” said Sharpless in his sobering statement. “The impact resulting from closure of these and perhaps more facilities will be difficult to reverse, and ultimately could result in years of spot or nationwide shortages of critical medical devices, which could compromise patient care.”
The acting commissioner went on to urge device manufacturers to perform inventory assessments and to alert them of potential shortages. The FDA says they will continue to work with device makers and healthcare institutions to triage services to other operating facilities or find alternative sources of much-needed medical devices.
They also reiterate that there are no viable alternatives to this method of sterilization yet. This could change as the deadline for submissions to the FDA’s summer innovation challenges for alternative sterilization approaches and ethylene oxide emission reduction strategies draws near.
Adding to the pressure on device manufacturers seeking to continue business-as-usual is the Environmental Protection Agency’s (EPA) review of the Clean Air Act, scheduled to be completed by March 2020. In the wake of environmental and health concerns, this could mean restricting the acceptable levels of ethylene oxide emissions by commercial facilities, including medical device sterilization plants. Industry trade lobby group AdvaMed (Advanced Medical Technology Association) had already voiced their concerns over the risks of such a rule, especially when there are no appropriate alternative options available.
If device manufacturers were not worried about their supply chains then, they ought to be now. The FDA will be holding a public advisory meeting in early November to discuss best strategies for encouraging innovation in medical device sterilization.
*Editor’s note: A previous version of this article inaccurately stated the reasons for the closure of the Illinois and Georgia Sterigenics facilities.








Join or login to leave a comment
JOIN LOGIN