In preeclampsia, safety for both mother and baby, including avoiding placental transfer, is a key factor in developing new therapies.
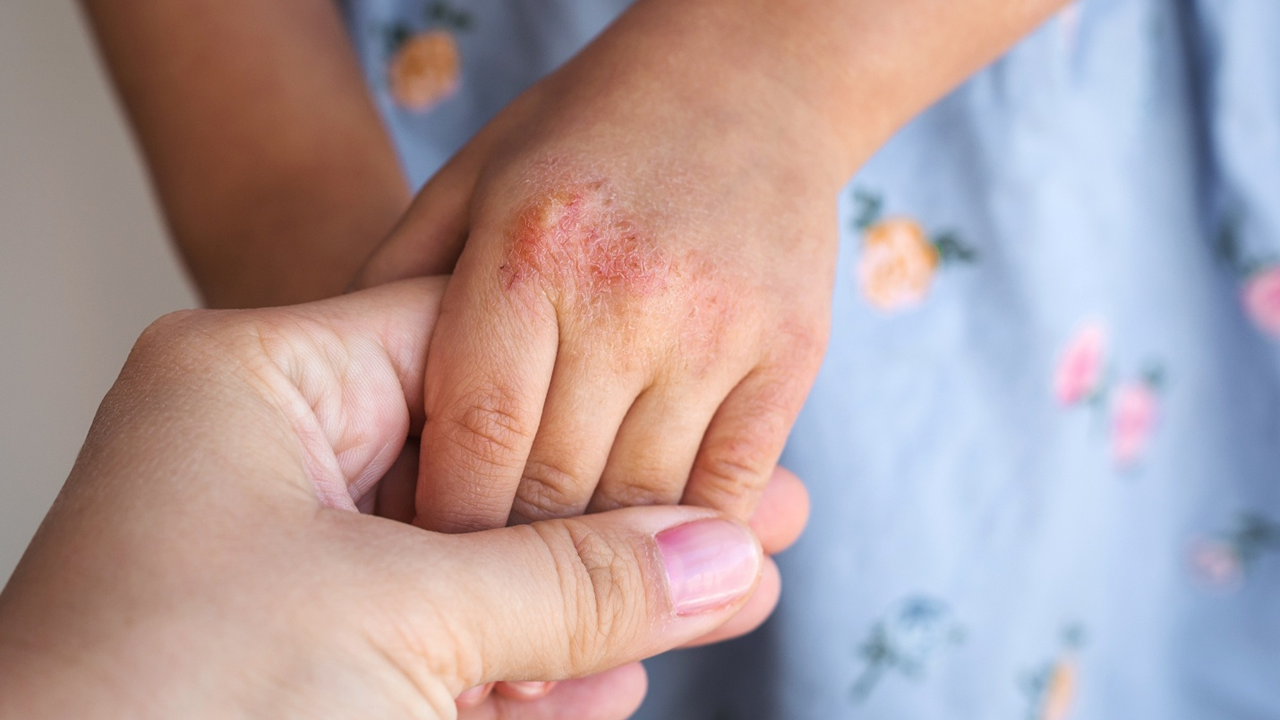
Preeclampsia, a hypertensive disorder driven in part by impaired placental blood flow, affects an estimated 3% to 8% of women in the US and remains a major cause of maternal and neonatal complications.

President and CEO
DiaMedica
DiaMedica Therapeutics is studying a recombinant form of tissue kallikrein in ischemic settings, where impaired blood flow plays a central role in disease pathophysiology.
DiaMedica is led by Rick Pauls, President and Chief Executive Officer, who has led the company since 2009. With prior experience spanning life sciences venture capital, finance and board leadership, he now oversees the company’s clinical and development strategy in stroke and hypertensive disorders of pregnancy.
In this Xtalks Clinical Edge interview, Rick spoke with Xtalks about why DiaMedica has chosen to focus on difficult ischemic diseases, the biological rationale for targeting the kallikrein-kinin pathway and how this approach is being translated into clinical studies in stroke and preeclampsia. He also discussed the practical challenges of developing therapies in areas with profound unmet medical need.
Targeting Diseases with Limited Options
DiaMedica’s focus on ischemic disease, Rick explained, grew out of a deliberate decision to work in areas where therapeutic progress has been limited, and treatment options remain few.
He pointed first to acute ischemic stroke, noting that no new drug has been approved since tissue plasminogen activator in 1996. A key factor in entering this space, he explained, was prior clinical experience in Asia with the same biological pathway. In China, a form of tissue kallikrein isolated from human urine is used in routine care, providing real-world insight into dosing, patient selection and clinical feasibility for the recombinant KLK1 program now in development.
“There hasn’t been a drug approved since 1996 with tPA for stroke,” Rick said. “In China, there’s the same protein isolated from human urine that today is treating close to a million patients a year.”
Read Xtalks Clinical Edge™ Issue 7
Xtalks Clinical Edge is a magazine for clinical research professionals and all who want to be informed about the latest trends and happenings in clinical trials. This magazine immerses you in a world where industry leaders, patient advocates and top researchers converge to provide the most insightful perspectives on clinical trials.
He said results from DiaMedica’s own trials later showed consistent reductions in blood pressure, which prompted the company to look toward hypertensive disorders of pregnancy. He described preeclampsia as a setting with long-standing treatment gaps and major unmet need, where improving maternal blood pressure control and extending gestation could affect both neonatal outcomes and time spent in intensive care.
“We came to preeclampsia. I mean, it’s a hypertensive disease of pregnancy, a very, very difficult indication in terms of just the lack of treatments that have been in development over the years,” Rick said. “So really just this passion of trying to go after these difficult diseases where there’s just a huge unmet medical need.”
— Rick Pauls, President & CEO, DiaMedica
The Kallikrein-Kinin Pathway & Focal Blood Flow
Rick described how their investigational recombinant form of tissue kallikrein is intended to act in ischemic tissue by engaging the kallikrein-kinin system.
In acute ischemic stroke, he said, a clot blocks perfusion to the penumbra, and if that obstruction is not removed with thrombolysis or mechanical thrombectomy, permanent tissue damage can occur. He noted that fewer than 20% of patients currently receive either intervention.
He then described what he sees as a distinguishing feature of the kallikrein-kinin pathway in ischemia. Tissue kallikrein is a naturally occurring protein, and he said that patients at risk for stroke and preeclampsia tend to have lower endogenous levels. In the ischemic penumbra, cells markedly upregulate bradykinin B2 receptors, but the ligand needed to activate them is deficient.
He said that by supplying recombinant KLK1, which generates bradykinin, the therapy is intended to activate these receptors and induce localized vasodilation, drawing blood into areas with compromised perfusion.
“You’ve got cells in the penumbra ischemic area, that have these bradykinin B2 receptors that are upregulated 35-fold, at least in animals. But what’s missing is the ligand bradykinin,” Rick said. “So our treatment… releases bradykinin, and then it attaches to where those receptors are.”
Turning to preeclampsia, Rick characterized the condition as one in which inadequate opening of the uterine spiral arteries limits delivery of oxygen and nutrients to the placenta.
Rick said DiaMedica’s clinical data have shown not only reductions in maternal blood pressure but also changes in Doppler-based measures of uterine artery resistance, specifically the pulsatility index, which reflects downstream blood flow.
“The more resistance, the less blood flow. So, by seeing a significant improvement in this marker, we think we can actually get more blood flow to the placenta.”
Demonstrating Safety in Pregnancy
Rick said the central challenge in developing therapies for preeclampsia is that trials must account for both maternal and fetal safety, noting that any off-target exposure to the fetus could have serious consequences. He explained that this was a key reason DiaMedica focused early on determining whether its recombinant KLK1 could cross the placental barrier.
“You’re dealing with two lives. And if you have some off-target effects that get to the baby, I mean, that could have profound effects,” Rick said. “So the size of our protein is about 26 kilodaltons, whereas the cutoff across the placental barrier is about 500 daltons.”
He described how this question was examined in a clinical study in pregnant women by measuring drug levels in maternal blood and in cord blood at delivery. According to Rick, the data showed detectable levels of the study drug in mothers, with no detection in the fetal circulation. The work was conducted in Cape Town, South Africa, at a clinical unit that had treated and dosed approximately 500 to 600 patients across different trials over the past three years, allowing the team to generate these measurements efficiently.
Rick also said that endogenous levels of tissue kallikrein are lower in women with preeclampsia, and lower still in severe disease, and described the program as a form of protein replacement.
He also referred to prior clinical use of related forms of the protein, isolated from pig pancreas and from human urine, which have been used in large patient populations in Japan and China. He added that DiaMedica has now dosed more than 300 patients across its own studies.
Selecting Patients & Endpoints in Ischemic Trials
One of the persistent challenges in both stroke and preeclampsia is that preclinical findings have often failed to translate into clinical benefit. In stroke, Rick explained, DiaMedica has tried to address this by grounding its program in extensive prior human experience with urinary kallikrein, along with input from practicing stroke neurologists, to help define which patient populations are most likely to respond and which are less likely to benefit.
“There’s close to a million patients being treated per year with the human urinary form, with 200 clinical papers published,” Rick said. “So for us, we have been able to really leverage what’s been working with this urine form, talking to stroke neurologists and been really able to dial in and identify a patient population that we think will be responders.”
With respect to preeclampsia, Rick noted that only a small number of clinical trials have been conducted in this indication to date. He said DiaMedica therefore began by focusing on symptomatic endpoints such as maternal blood pressure, and then on exploratory vascular markers, including Doppler evidence of reduced resistance in the uterine arteries, as potential indicators of improved placental perfusion.
“That’s where we are seeing early signs of dilation of the intrauterine arteries,” he said. “So we think that together this should help to keep the babies growing larger in the mother for a longer period of time, which should result in larger, healthier babies that should see fewer neonatal events, fewer days in the NICU.”
— Rick Pauls, President & CEO, DiaMedica
Imaging, Diagnostics & Earlier Intervention
Rick said imaging remains central in acute ischemic stroke, while current pharmacologic treatment is constrained by time. He noted that tissue plasminogen activator must be administered within a four-and-a-half-hour window, after which therapeutic options become far more limited.
“CT scans work very well, and so that’s really helping to identify these patients,” Rick said. “The challenge for stroke is that what we have today, tPA, which is effective, has to be given within a four-and-a-half-hour window.”
He then described newer digital tools that support faster triage and specialist input, particularly when patients first present to community hospitals. He said these systems allow local teams to consult with stroke neurologists to determine whether a patient is eligible for mechanical thrombectomy and should be transferred to a comprehensive stroke center, or managed locally if not.
In preeclampsia, Rick said that while certain diagnostic tests can enable earlier identification of the condition, this alone does not address the therapeutic gap, given the limited range of drugs that can be safely used during pregnancy. He noted that some agents previously explored for blood pressure control were constrained by placental transfer.
“Even if they can tell a patient that they’ve got preeclampsia, they’re really limited in treatment options,” Rick said.
Gestational Age, Neonatal Outcomes & Health System Burden
Rick explained that babies born very prematurely may require months of intensive neonatal care and can face long-term complications, and that delaying delivery by several days could influence both immediate outcomes and downstream resource use.
“If a baby is born at, for example, 28 or 29 weeks, that baby could be in the NICU for six months,” he said. “If that baby’s born even a few weeks earlier, that baby could be in the NICU for a year.”
He said that even modest extensions in gestation could meaningfully affect outcomes. Based on discussions with obstetricians, Rick noted that keeping the fetus in utero for several additional days could influence birth weight, early morbidity and the duration of intensive care.
“Even four to five days… can have a profound impact in terms of the baby’s outcomes.”
Disparities in Preeclampsia Outcomes
Addressing equity, Rick shifted to who is most affected by this burden. He noted that preeclampsia occurs at higher rates among Black, American Indian and Alaska Native women and other minority populations.
He framed earlier and more effective intervention in these groups as a potential way to influence outcomes in a setting where disease burden is disproportionately high. In his view, approaches that help delay delivery and extend gestation could be particularly relevant in populations that experience higher rates of severe disease and its complications.
The Drug Development Landscape in Ischemic Disease
Looking more broadly at the clinical research environment, Rick reflected on how few therapies are currently being developed for ischemic conditions such as stroke and preeclampsia.
He contrasted this with areas like oncology and metabolic disease, where large pipelines and numerous late-stage programs exist, and described the relative scarcity of active development in ischemia as both a challenge and a motivator.
“For both stroke and for preeclampsia, there really is just a small handful of companies that are even in development… It’s just this massive need. And unfortunately, there’s just been a real lack of drugs in development today.”










Join or login to leave a comment
JOIN LOGIN