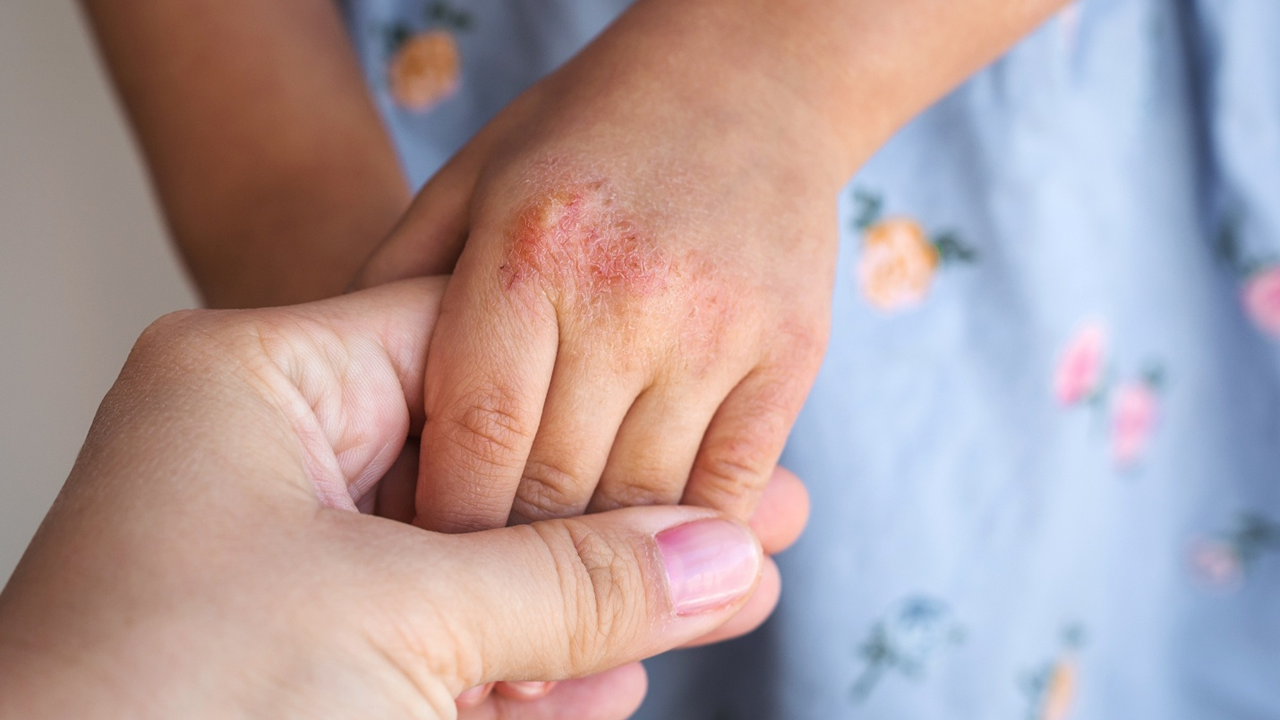
World Obesity Day 2026 is recognized on March 4. The scale of the challenge is clear. In the US, more than 1 in 5 children and adolescents ages two to 19 were living with obesity between August 2021 and August 2023, based on recent CDC estimates. This figure includes 7% with severe obesity, a condition associated with higher risks for cardiovascular and metabolic complications even at a young age.
In response, this year’s World Obesity Day focuses on the theme “eight billion reasons to act,” highlighting children and communities most affected by rising obesity rates.
Forecasts indicate that by 2035, about four billion people worldwide — roughly half the global population — could be living with overweight or obesity.
Childhood Obesity on the Rise
Rates of overweight and obesity among school-aged children have increased steadily over the past several decades. In the US, national survey data show that obesity prevalence among children and adolescents rose from single-digit levels in the 1970s to 21.1% across August 2021 to 2023, with increases observed across all pediatric age groups.
Childhood obesity often continues into adulthood and is associated with a higher risk of non-communicable diseases, including type 2 diabetes, cardiovascular disease and certain cancers. Clinicians are also reporting earlier signs of metabolic complications, such as insulin resistance and elevated blood pressure, raising concerns about long-term health outcomes and increasing strain on healthcare systems.
Children living with obesity may also experience stigma, bullying and discrimination, which can discourage engagement with healthcare and supportive services.
Obesity as a Systems Issue
Obesity is shaped by food environments, socioeconomic conditions and public policy, making population-level action central to prevention.
In March 2025, Pakistan became the 64th country to implement a national ban on industrially produced artificial trans fats, which are linked to higher risks of heart attacks and strokes. The regulation now protects more than 240 million people and reflects a broader global effort to reduce cardiovascular risk through changes to the food supply rather than relying solely on downstream treatment.
GLP-1 Drug News: Treatment Options and Delivery Models
In 2023, spending on GLP-1 receptor agonists, including semaglutide- and tirzepatide-based drugs, exceeded $71 billion in 2023, with products such as Ozempic, Wegovy and Mounjaro accounting for the majority of total spending on the drug class.
The visibility of GLP-1 therapies in mainstream media, such as public discussions by figures such as Oprah Winfrey and Serena Williams, has further increased consumer awareness and, in some markets, contributed to higher patient demand for weight-management care.
At the same time, treatment options for obesity and related metabolic conditions are evolving rapidly.
One key area of focus is the development of oral therapies aimed at reducing reliance on injections and improving long-term adherence. In February 2026, Novo Nordisk announced a partnership with Vivtex to develop next-generation oral biologic medicines for obesity, diabetes and related conditions. The collaboration seeks to improve the oral absorption of peptide- and protein-based drugs typically delivered by injection, which could simplify treatment and broaden access over time.
Phase III trial data published in The Lancet showed Eli Lilly’s investigational oral GLP-1 receptor agonist orforglipron demonstrated greater reductions in blood sugar and body weight than oral semaglutide in adults with type 2 diabetes. Participants receiving the higher dose of orforglipron achieved more than 9% average placebo-adjusted weight loss over 52 weeks, along with improvements across multiple cardiometabolic risk factors. Regulatory submissions are underway in more than 40 countries, with potential regulatory decisions for obesity expected later in 2026.
Broader Metabolic Innovation Beyond Weight Loss
Some emerging therapies are also targeting metabolic dysfunction in populations where obesity overlaps with other chronic diseases.
In February 2026, GSK shared plans to acquire 35Pharma, adding an investigational activin signaling inhibitor to its pipeline for pulmonary hypertension. Early clinical findings suggest potential metabolic benefits, including selective weight loss and improved insulin sensitivity. These effects could become relevant given the high prevalence of obesity and insulin resistance among patients with pulmonary hypertension.
Beyond drug-based approaches, employers and health plans are also exploring digital models for metabolic care. In August 2025, Twin Health reported new investment and outcomes data for its AI-enabled “digital twin” platform designed to support diabetes and weight management through personalized metabolic monitoring.
If you want your company to be featured on Xtalks.com, please email [email protected].











Join or login to leave a comment
JOIN LOGIN