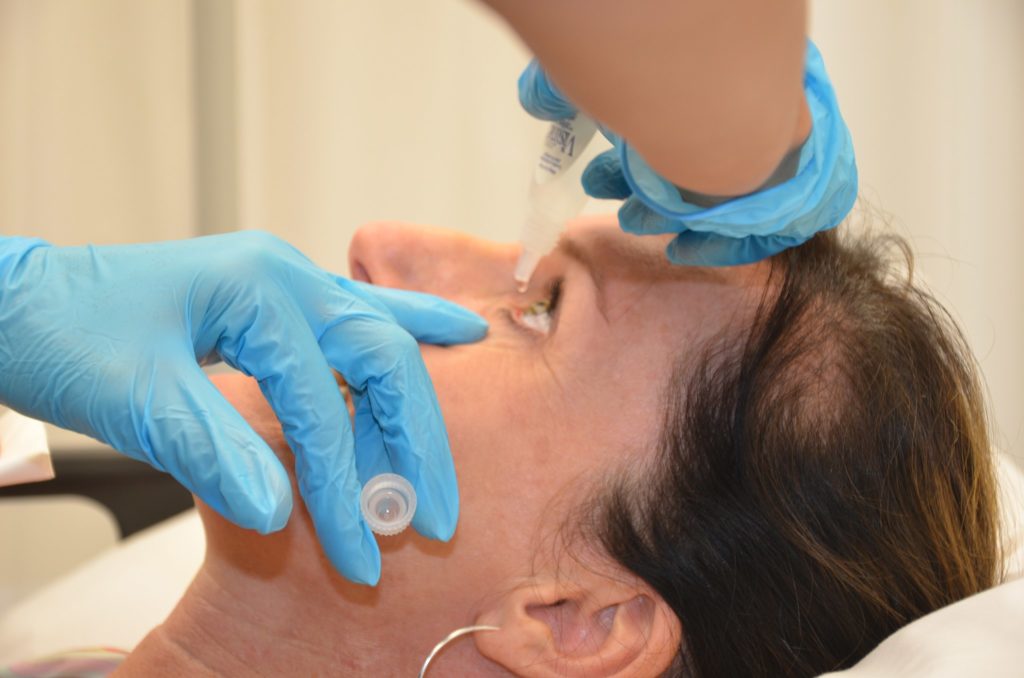
Anyone who uses eye drops knows the frustrations of conventional eyedroppers: too much of the ophthalmic medication is often dispensed, causing eye irritation and more frequent trips to the pharmacy for refills. Now, researchers at New York Eye and Ear Infirmary of Mount Sinai have developed an eyedropper that delivers a microdose of medication.
Patients who rely on daily application of medicated eye drops to treat conditions such as glaucoma or dry eye could benefit the most from this new eyedropper, as such drugs are often expensive. The researchers presented the details of the new device at AAO 2017, the 121st Annual Meeting of the American Academy of Ophthalmology.
The drop size dispensed by a conventional eyedropper contains up to 5 times more liquid than can be held by the eye. Excess medication can cause localized side effects such as redness and irritation, and in the case of some drugs, may have effects on other parts of the body such as the heart’s rhythm.
In comparison to conventional eyedroppers, the researchers’ microdosing device was capable of dispensing four times less liquid while still achieving the desired effect of the drug. This smaller dose reduced the eye’s exposure to the drug – and any preservatives included in the medication – by up to 80 percent, resulting in fewer side effects.
Because the device delivers microliter doses of eye drops in just 80 milliseconds, it reduces blinking and tearing which can dilute the effects of the medication. By reducing side effects and improving user experience, the microdosing device could even improve medication adherence among patients.
“We believe that we have developed a viable 21st-century microdosing technology to transform the 100-year old eyedropper paradigm with modern, high-precision smart technology,” said Dr. Tsontcho Ianchulev, professor of ophthalmology at the Icahn School of Medicine at Mount Sinai.
In their evaluation of the microdosing system, the researchers administered a drug designed to dilate the pupils to a group of patients. Compared to the conventional eyedropper, the precision microdosing produced the same pupil dilation effect.
What’s more, only eight percent of patients given the microdose reported negative side effects, compared to 66 percent of patients treated using the conventional eyedropper method. Those patients also showed lower levels of the drug in their blood, suggesting that most of the medication is absorbed by the eye.
According to Ianchulev, the team has plans to conduct further clinical trials in the next year to assess the safety and efficacy of microdosing. If results from these studies continue to be favourable, the team says that microdose versions of ophthalmic medications could be on the market by 2020.










Join or login to leave a comment
JOIN LOGIN