A decade after the human papillomavirus (HPV) vaccine was introduced in the UK, the NHS has decided to extend the offer of vaccination to young boys as well as girls. The Joint Committee on Vaccination and Immunisation (JCVI) was the catalyst behind the decision as they found that including boys in the vaccination program against the virus would be cost-effective.
“Any vaccination program must be firmly grounded in evidence to ensure that we can get the best outcomes for patients, but as a father to a son, I understand the relief that this will bring to parents,” said public health minister Steve Brine.
The governments of Scotland and Wales have also followed suit and decided to take the recommendation of JCVI.
At the moment, the NIH will cover the cost of the HPV vaccine for girls under the age of 18 and the vaccine is most often administered to girls between he ages of 12 and 13. Since HPV is a sexually-transmitted disease, the goal of this vaccination program is to provide girls with protection before they become sexually active.
While HPV infection has been most commonly associated with a risk of developing cervical cancer, it’s also been linked to other cancer types include penile, anal, oral and throat. For this reason, the HPV vaccine will also be offered to boys to prevent them from contracting the virus themselves and spreading it to others.
According to Public Health England, the vaccination program has already been a success in the UK where the prevalence of two of the most common, disease-causing strains of HPV has plummeted by 80 percent.
“Almost all women under 25 have had the HPV vaccine and we’re confident that we will see a similarly high uptake in boys,” said Mary Ramsay, head of immunisations at Public Health England.
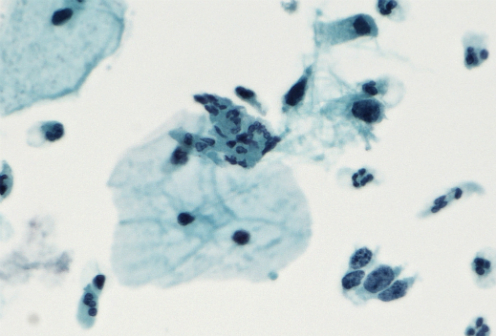
The UK isn’t the only nation that’s seen a public health benefit since the implementation of the HPV vaccination program; a recent study of the first birth cohort of girls in Denmark to be given the HPV vaccine found that these women had a 40 percent lower risk of developing abnormal cervical cells – known as dysplasia.
“This means that fewer women have to be referred to a gynaecologist for further examination and have a tissue sample taken. Eventually we also expect fewer to fall ill,” said Lise Thamsborg, first author of the study.
Danish health authorities have also lowered the vaccination age for girls in the country from 15 to 12, which the researchers believe will lead to an even greater reduction in dysplasia. The country does offer vaccination to boys as well, according to the country’s public health department.







Join or login to leave a comment
JOIN LOGIN