This week marked World Antimicrobial Awareness Week (WAAW), a global campaign celebrated every year to help raise awareness and understanding of antimicrobial resistance (AMR).
The theme of this year’s World Antimicrobial Awareness Week is “Preventing Antimicrobial Resistance Together,” which highlights the need for collective action in the fight against AMR.
The slogan is a call for collaborative efforts to address AMR using a One Health approach. It is led by the Food and Agriculture Organization of the United Nations, the World Organization for Animal Health and the World Health Organization (WHO). The goal is to encourage best practices among the public, One Health stakeholders and policymakers to address the issue of AMR.
In 2021, the WHO identified AMR as one of the top ten global public health threats facing humanity.
AMR is often called the “silent pandemic” that has the potential to affect both human and animal well-being, the environment, food safety as well as economic growth and development.
According to the WHO, the silent pandemic leads to at least 1.3 million human deaths every year.
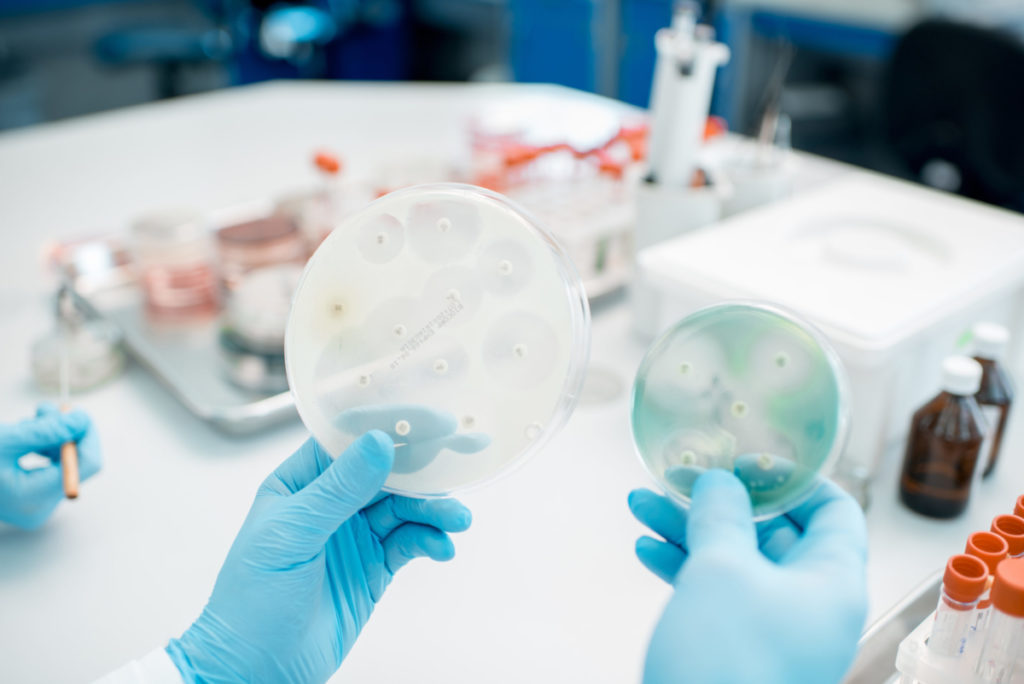
There are several strains of bacteria that have developed resistance to different types of antibiotics — these include MRSA (methicillin-resistant Staphylococcus aureus) Clostridium difficile (C. diff) and the bacteria that cause multi-drug-resistant tuberculosis. And the number of resistant strains is growing.
To learn more about AMR and the challenges in fighting it, Xtalks spoke with Jessica Blavignac, Director of Scientific and Medical Affairs at bioMérieux Canada, a global diagnostic solutions company, and Janelle Jiminez from One Health where she manages the AMR One Health Consortium involving individuals doing AMR research in Alberta, Canada.
Currently, in Canada, 26 percent of infections are resistant to antibiotics that have been traditionally used to treat them. The health and economic implications of this are staggering. Blavignac said if trends continue, by 2050, this could cause up to 15 deaths per day, a loss of $1.4 billion to the healthcare system and even translate to a $396 billion loss in GDP.
She said this is alarming because if this is the state in a high-income country like Canada, “if you transpose that to a country that has less resources, the impact will be far more detrimental.”
Causes of Antimicrobial Resistance
While the overuse of antibiotics in recent years has been one of the primary contributors to AMR, there are a number of other factors at play. The list includes:
- Antibiotic misuse/overuse
- Antibiotic use in animal agriculture
- A lack of/insufficient infection control measures (i.e. basic hand washing/hand hygiene)
- Transport of animals, food and other products globally that can carry pathogens
- Absence of uniform infectious disease surveillance programs across different regions
- Lack of coordinated global response to infectious disease outbreaks
The overuse of antimicrobials promotes resistance and can lead to the evolution of “superbugs.” The worry is that if enough of these superbugs arise, or if they develop multidrug resistance, current antibiotics may not be effective against them. Clinicians, patients and policymakers must therefore be vigilant and strategic in the use of antibiotics, ensuring they are only used for infections caused by bacteria and not viruses, for example.
Jiminez said there needs to be an understanding that “not all bugs need drugs. People feel that if they’re sick, they need to be given something to treat it and that using their own immune system [in the case of clearing a viral infection, for example] is not really an option. If you have a common cold or any kind of viral infection, you would need an antiviral or you clear it naturally.”
Moreover, Jiminez said that in some countries, there aren’t any restrictions against prescribing antibiotics and there is even access to them over the counter.
The key to improving awareness around better antibiotic use is education, and also the use of appropriate diagnostic tools to quickly screen for the type of infection a patient may have.
“If it is a bacterial, fungal infection, viral or parasitic infection, then you know your course of treatment rather quickly as opposed to exposing the patients to an antibiotic that is broad scale or that’s empirical,” explained Blavignac.
The use of antibiotics in animal agriculture is also a concern. However, the conversation around that should be more nuanced as there are ethical issues with not treating sick animals.
There also needs to be a better understanding of how related the environment and agriculture are, as antibiotics are used in animal agriculture, animals that we use for food. With antibiotics in the food chain, they also seep into the environment, as does antibiotic-containing wastewater from hospitals and biopharmaceutical production, contributing to the spread of AMR.
Therefore, Jiminez said “it is not just up to one discipline to focus on [the problem of AMR] but we all need to work together [as] everything is interconnected.”
Other factors contributing to AMR include poor infection prevention and control practices that include basic hand washing/hand hygiene, and insufficient diagnostic tools for rapid and reliable detection of resistance.
Blavignac said the absence or limited access to vaccines globally is another problem, in addition to a lack of global uniformity or even a complete lack of disease surveillance programs and coordinated response to infectious diseases across different regions. “Being able to detect emerging pathogens or signals of a pandemic could really make a difference in our ability to control and prevent infections,” added Blavignac.
While similar, coordinated practices should be applied to curb the spread of infectious pathogens, developing countries may have limited resources and thus may be at a higher risk of resistance than North America, for example.
And globalization also has an impact as people, animals and food products travel across continents, which can spread pathogens very quickly. But at the end of the day, “we have a civil duty to help one another out,” said Blavignac.
Related: Why Antimicrobial Resistance is a Silent Pandemic – Xtalks Life Science Podcast Ep. 26
Approaches and Solutions to Tackle AMR
Education and delivering clear information are an integral part of dealing with AMR. And the approach must be multi-faceted and include multiple players, which ties into this year’s World Antimicrobial Awareness Week’s theme of preventing antimicrobial resistance together.
Jiminez says it’s a matter of getting everybody on board and getting the information out there, and to perhaps “have a campaign that’s hopefully as big as breast cancer awareness, MS or other ones that more people know about globally.”
However, a challenge seen during the COVID-19 pandemic has been getting the right information out to people while dealing with misinformation.
Jiminez also highlighted the importance of having more partnerships between low- and middle-income countries as well as first world countries. This would help disseminate information in a cohesive and uniform manner, so that people everywhere are getting the right information collectively.
And globally recognized events and awareness campaigns like World Antimicrobial Awareness Week are more of what we need. The key is also to have training opportunities where multiple organizations and disciplines can come together to learn from one another and then spread the word, said Jiminez.
In “Preventing AMR Together,” the together part is the most important because it’s a global issue. “We really need to be reaching out to other countries and connecting and collaborating more with low- and middle-income countries where this is also a big issue to make sure that we’re all on the same page.” And the togetherness is also about applying the same techniques and having the same outcomes, she said.
Fostering connectivity and collaborations between different disciplines is also important because oftentimes there is a lack of understanding between different areas. For example, through her work, Jiminez said a challenge she’s noticed is that even though medical doctors, veterinarians, environmentalists and scientists may all be working together on AMR, a lot of us still have differing views and how AMR works in other fields.
“All of these disciplines really need to be very perceptive of how other industries or other disciplines work, and work together with that.”
For example, there is a public understanding and perception that antibiotics are overused in raising beef cattle. However, from an animal welfare perspective, Jiminez said we cannot not give them antibiotics because without them, they get really sick and are in a lot of pain so it is not ethically fair for the animal.
A multidisciplinary approach involves bringing together different disciplines and fostering understanding between them. Therefore, a true multidisciplinary understanding of AMR has to involve an understanding of AMR in different disciplines and the challenges that they face.
Having governments on board is also important. Jiminez explained how at AMR One Health Consortium, their action plan is to directly work with the University of Calgary to conduct environmental scans and surveys to help figure out the best course of action going forward, which governments are picking up on and investing more money into AMR research.
The goal is to also have government funded initiatives in smaller countries and bring together the initiatives through summits that involve countries coming together to talk about what they’re going to do and come up with ways to combat AMR going forward.
Take Home Message
AMR will affect everyone is Jiminez’s take home message. “A lot of people think that it doesn’t, [or] it hasn’t affected me in my life thus far, so I don’t have to worry about it, but people need to realize that it will, if it has not already, eventually affect you in some way.”
For Blavignac, walking in the same direction is vital to having an impact. And this is important because “we all have to apply the same practices in order to be able to curb the development of resistance.”
The theme of togetherness in preventing AMR will be a constant one moving forward against AMR. Importantly, this must involve collaborative action across disciplines and across countries because AMR is a global issue that will impact almost all industries, disciplines and people worldwide.










Join or login to leave a comment
JOIN LOGIN